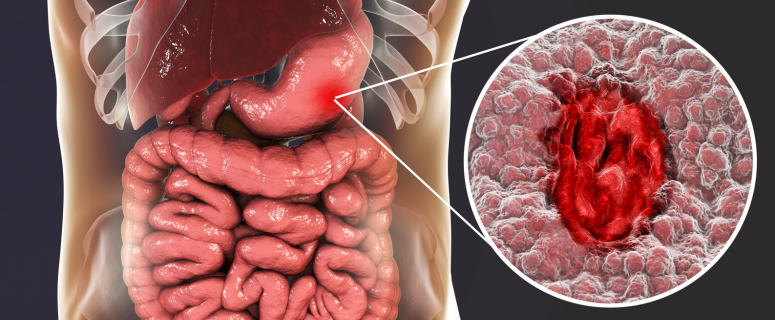
Ulcerative colitis (UC) is a chronic inflammatory bowel disease characterised by inflammation and ulceration of the colon and rectum. Diet cannot cure UC — it is a disease requiring medical management — but what you eat directly influences symptom severity, flare frequency, nutritional status, and quality of life. Eating the wrong foods during a flare can significantly worsen symptoms. Eating strategically during remission can help maintain it.
This guide provides a clinically grounded 7-day meal plan for UC, explains the difference between eating during a flare versus in remission, covers the medications most commonly used for UC and their nutritional interactions, and gives you the evidence base behind each dietary recommendation.
Pharmacist’s Perspective — Faryal Faisal, PharmD
Ulcerative colitis management involves some of the most clinically significant drug-nutrient interactions I encounter in pharmacy practice — and they are almost never discussed in general diet guides for UC.
The most important one: patients on mesalamine, azathioprine, or corticosteroids for UC are at significantly elevated nutritional risk that goes beyond what food alone can address. Corticosteroids — prednisolone, budesonide — deplete calcium, vitamin D, potassium, and magnesium with prolonged use and directly cause bone loss. Patients on long-term corticosteroids need calcium and vitamin D supplementation alongside dietary sources — not instead of them. If you are on corticosteroids for more than three months and have not discussed bone health supplementation with your physician, raise it at your next appointment.
Azathioprine and 6-mercaptopurine deplete folate. Mesalamine can reduce folate absorption. Both folate deficiency and UC independently increase colorectal cancer risk — patients on these medications should ensure adequate folate intake from food and discuss folic acid supplementation with their physician.
Biologics (infliximab, adalimumab, vedolizumab) used in moderate-to-severe UC do not have specific nutritional depletions, but the immunosuppression they cause means food safety is critically important — undercooked meat, unpasteurised dairy, and raw fish carry higher infection risk in immunosuppressed patients.
Finally — iron deficiency anaemia is the most common extraintestinal complication of UC, present in up to 74% of patients at some point. If you are fatigued, pale, or breathless and have UC, ask your physician for a full blood count and iron panel.
— Faryal Faisal, PharmD, Start Being Healthy
What Is Ulcerative Colitis?
Ulcerative colitis is a chronic immune-mediated inflammatory disease of the large intestine (colon) and rectum. Unlike Crohn’s disease — which can affect any part of the gastrointestinal tract — UC affects only the colon and rectum, with inflammation typically starting in the rectum and extending continuously upward.
UC is characterised by periods of active disease (flares) and periods of reduced or absent symptoms (remission). The pattern of eating needs to differ significantly between these two phases — what is appropriate during remission can worsen a flare, and what is necessary during a flare is unnecessarily restrictive during remission.
Core symptoms during a flare:
- Frequent loose or bloody stools
- Urgency and abdominal cramping
- Fatigue — often from blood loss, anaemia, and systemic inflammation
- Weight loss during prolonged flares
- Reduced appetite
Prevalence and severity: UC affects approximately 5 million people globally. Disease severity ranges from mild (fewer than four stools daily, minimal blood) to moderate to severe (more than six bloody stools daily, systemic symptoms). Dietary management differs by disease severity.
The Critical Distinction: Eating During a Flare vs. in Remission
This is the most important clinical point in this entire guide — and the one most general UC diet articles miss entirely.
During a flare — the inflamed, ulcerated colon cannot tolerate the same foods it handles well in remission. High-fibre foods, raw vegetables, whole grains, legumes, nuts and seeds, and spicy foods can all increase stool frequency, worsen cramping, and aggravate the inflamed mucosa. During an active flare, the priority is symptom management through a low-residue, low-fibre, easily digestible eating pattern — not nutritional optimisation.
During remission — the colon has healed and can tolerate a much wider variety of foods. The dietary priority shifts to nutritional rehabilitation (correcting deficiencies accumulated during the flare), supporting gut microbiome health, and following an anti-inflammatory eating pattern that may help maintain remission. The 21-Day Anti-Inflammatory Diet Plan approach becomes more applicable during remission.
The 7-day meal plan in this guide is designed for mild UC or remission. If you are currently experiencing an active moderate-to-severe flare with frequent bloody stools, systemic symptoms, or significant weight loss, contact your gastroenterologist. A severe flare requires medical management — not just dietary adjustment.
What the Clinical Evidence Shows
2023 systematic review and meta-analysis — dietary interventions in UC — 14 RCTs were included. Results indicated higher clinical response, remission, and endoscopic remission rates in diet-treated groups compared to controls. Pooled analysis favoured dietary intervention for sustaining clinical remission. (Herrador-López M, et al., Nutrients, 2023 — PMC: 10574654)
2023 systematic review — role of diet in UC — 27 clinical trials and RCTs published between 2010 and 2023 were reviewed. Low-FODMAP, Mediterranean, and anti-inflammatory dietary patterns appeared to improve symptoms and overall quality of life in UC patients. Anti-inflammatory diet combined with faecal microbiota transplantation outperformed standard medical therapy for clinical response and remission in one included study. (Abbas et al., Cureus, 2023 — PMC: 10284595)
2024 AGA Clinical Practice Update — diet and IBD — The American Gastroenterological Association’s expert review found no single diet consistently decreases UC flare rates, but a diet low in red and processed meat may reduce UC flares. The AGA recommends individualised dietary assessment and avoiding unnecessarily restrictive diets that worsen nutritional status. (Hashash JG, et al., Gastroenterology, 2024 — PubMed: 38276922)
2023 review — nutritional therapies in IBD — Mediterranean diet, specific carbohydrate diet, and low-FODMAP approaches all show evidence of benefit in IBD. The Mediterranean diet has the broadest evidence base for anti-inflammatory effects and nutritional completeness. (Reznikov EA, Suskind DL, Nutrients, 2023 — PMC: 9920576)
The honest evidence picture — no single dietary approach has been proven to induce or maintain UC remission consistently across all patients. Diet is an important adjunct to medical therapy, not a replacement. Individual trigger foods vary significantly between patients. The evidence most strongly supports: avoiding ultra-processed foods and red/processed meats, following a generally anti-inflammatory eating pattern during remission, and using a low-residue approach during active flares.
Foods to Eat With Ulcerative Colitis
During remission — generally well tolerated
Lean proteins — baked or grilled chicken, turkey, fish (particularly salmon for omega-3 anti-inflammatory effects), eggs, and tofu. Protein is essential for mucosal repair and maintaining lean mass during a disease that frequently causes weight loss. Aim for 1.2–1.5g of protein per kg of body weight — higher than general population recommendations due to increased protein losses in UC.
Well-cooked vegetables — cooking significantly reduces the fibre and fermentable content of vegetables, making them better tolerated. Carrots, courgette, sweet potatoes, squash, parsnips, and green beans are among the most tolerated vegetables. Peel vegetables before cooking to further reduce fibre load. Raw vegetables are better tolerated during remission than during flares.
Low-fibre grains — white rice, oats, white bread, and refined pasta are more easily digestible than whole grains. Whole grains can be reintroduced gradually during stable remission as tolerance allows — monitor individual response.
Eggs — one of the most UC-friendly protein sources. High-quality protein, easily digested, no fibre, and highly versatile. Hard-boiled, scrambled, or poached eggs are all well tolerated.
Salmon and other fatty fish — the omega-3 fatty acids EPA and DHA in fatty fish have documented anti-inflammatory effects in IBD. A meta-analysis found omega-3 supplementation reduced the relapse rate in UC patients. Two to three servings per week during remission is supported by evidence.
Low-lactose or lactose-free dairy — many people with UC have secondary lactose intolerance, particularly during flares. Lactose-free yogurt, kefir, and lactose-free milk are generally well tolerated. Plain yogurt and kefir also provide probiotics that support gut microbiome health.
Probiotics and fermented foods — the gut microbiome is significantly dysbiotic in UC. Probiotic supplementation (particularly VSL#3, which has the strongest IBD-specific evidence) and fermented foods including kefir and yogurt with live cultures may support remission maintenance. Discuss probiotic supplementation with your gastroenterologist.
Bananas and peeled fruits — bananas, tinned peaches in juice, applesauce, and peeled apples are among the most tolerated fruits. Avoid high-fructose fruits and dried fruits during flares.
Healthy fats — extra-virgin olive oil, avocado, and small amounts of nut butters provide anti-inflammatory fats and calories for weight maintenance. UC patients are at risk of unintentional weight loss.
Foods to Avoid With Ulcerative Colitis
Individual triggers vary between patients — what worsens symptoms in one person may be tolerated by another. The following are the most consistently problematic food categories across the evidence base.
During flares — avoid or significantly restrict
High-insoluble-fibre foods — raw vegetables, whole grains, bran, nuts and seeds, legumes, and corn. Insoluble fibre increases stool bulk and intestinal motility — both problematic during a flare when the colon is inflamed and motility is already increased.
Spicy foods and hot sauces — capsaicin directly stimulates intestinal motility receptors and can significantly worsen cramping and diarrhoea during a flare.
Dairy products (if lactose intolerant) — secondary lactose intolerance is common during active UC. Avoid lactose-containing dairy during flares and reintroduce gradually during remission.
Alcohol and caffeine — both increase intestinal motility and can worsen diarrhoea. Coffee, energy drinks, and alcohol should be reduced or eliminated during flares.
Carbonated beverages — increase intestinal gas and bloating, worsening abdominal discomfort.
High-fat fried foods — fat slows gastric emptying but stimulates the gastrocolic reflex, increasing urgency and stool frequency in UC.
Sorbitol and artificial sweeteners — found in sugar-free gum, candies, and some diet products. Poorly absorbed and can cause osmotic diarrhoea.
During remission and long term — reduce or eliminate
Ultra-processed foods — strong evidence links ultra-processed food consumption with increased UC flare risk and worse disease outcomes. A 2021 prospective study found high ultra-processed food intake was associated with significantly higher risk of IBD development and flare.
Red and processed meats — the 2024 AGA Clinical Practice Update specifically notes that a diet low in red and processed meat may reduce UC flares. Processed meats (bacon, sausage, deli meats) contain nitrates and advanced glycation end products that promote colonic inflammation.
Refined sugar and sugary beverages — promote gut dysbiosis and inflammatory signalling in the colon. A diet high in added sugar is associated with worse IBD outcomes in multiple studies.
UC Medications and Nutritional Interactions
This section is critical and almost never covered in UC diet guides. Faryal’s PharmD background makes this the most distinctive section of this article.
Corticosteroids (prednisolone, budesonide)
Used for inducing remission during moderate-to-severe flares. Cause significant nutritional depletions with prolonged use:
- Calcium and vitamin D depletion – bone loss and osteoporosis risk. Supplement with 1,000–1,200mg calcium and 800–1,000 IU vitamin D daily during and after corticosteroid courses. Discuss with your physician.
- Potassium depletion – include potassium-rich foods: bananas, sweet potatoes, white beans, and avocado.
- Magnesium depletion – include magnesium-rich foods: cooked spinach, pumpkin seeds, and dark chocolate (if tolerated).
- Increased appetite and blood glucose – corticosteroids increase appetite and can cause steroid-induced hyperglycaemia. Focus on low-GI carbohydrates and portion control during corticosteroid courses.
- Weight gain – common with prolonged courses. Use our Calorie Calculator to understand maintenance calories and avoid excessive weight gain during steroid treatment.
Azathioprine and 6-Mercaptopurine
Immunosuppressants used for maintenance of remission:
- Folate depletion – both drugs interfere with folate metabolism. Ensure adequate dietary folate (dark leafy greens, legumes, fortified foods) and discuss folic acid supplementation (typically 5mg weekly) with your physician.
- Increased infection risk – ensure all meat and fish is thoroughly cooked. Avoid unpasteurised dairy and raw shellfish.
- Nausea – a common side effect, particularly at initiation. Taking azathioprine with food significantly reduces nausea.
Mesalamine (5-ASA)
First-line maintenance therapy for mild-to-moderate UC:
- Folate absorption reduction – mesalamine can reduce folate absorption in the gut. Ensure adequate dietary folate and discuss supplementation with your physician.
- Generally well tolerated nutritionally – fewer significant drug-nutrient interactions than immunosuppressants or biologics.
Biologics (infliximab, adalimumab, vedolizumab, ustekinumab)
Used for moderate-to-severe UC unresponsive to other treatments:
- Immunosuppression and food safety – biologics significantly suppress immune function. Follow strict food safety protocols — avoid undercooked meat, raw fish (no sushi), unpasteurised dairy, and sprouts.
- No specific nutritional depletions – biologics do not cause the same nutritional losses as corticosteroids or antimetabolites, but nutritional status monitoring is still important given the severity of disease typically requiring biologic therapy.
Iron supplementation
Iron deficiency anaemia affects up to 74% of UC patients at some point. Oral iron supplementation can worsen GI symptoms in UC — intravenous iron infusion is often preferable for patients with active disease or significant anaemia. Discuss the route of supplementation with your gastroenterologist. Dietary iron from well-cooked red meat (in remission, in moderation), fortified cereals, and legumes supports iron status alongside supplementation.
7-Day Meal Plan for Ulcerative Colitis
This plan is designed for mild UC or remission. Adjust portion sizes based on your caloric needs using our Calorie Calculator. If any food worsens symptoms, remove it and consult your dietitian.
Day 1 — Setting the Tone for a Gut-Friendly Week
Breakfast: Microwaved old-fashioned oats with lactose-free milk, cinnamon, and cooked diced apples. Oats provide soluble fibre (beta-glucan) which is generally well tolerated in UC and supports gut microbiome health.
Lunch: Baked chicken seasoned with herbs, served with roasted carrots drizzled with olive oil and steamed white rice. Lean protein, cooked vegetables, and low-fibre grain — the UC-friendly foundation.
Dinner: Baked salmon with lemon juice, garlic, and pepper, served with peeled and baked summer squash and green beans seasoned with olive oil and garlic. Omega-3 from salmon is one of the most evidence-backed anti-inflammatory additions for UC.
Snacks: Small tin of tuna, peaches canned in water or juice, applesauce, hard-boiled egg.
Day 2 — Lean Proteins and Easily Digestible Grains
Breakfast: Plain lactose-free nonfat Greek yogurt topped with melted nut butter and a small amount of freshly squeezed juice. Greek yogurt provides protein and probiotics.
Lunch: Leftover baked salmon served cold with reheated sweet potatoes and green beans. Batch cooking is essential for UC management — energy levels are often reduced and having ready meals prevents falling back on processed foods.
Dinner: Harvest soup — pureed roasted red peppers, sweet potatoes, apples, and carrots — with toasted white bread and baked chicken. Pureed soups are particularly well tolerated during UC because the fibre structure is broken down.
Snacks: Hard-boiled egg with pears canned in juice; raspberries and lactose-free plain yogurt.
Day 3 — Dairy Alternatives and Soft Foods
Breakfast: Sweet potato toast topped with scrambled eggs and a small amount of cheese if tolerated. Sweet potato provides beta-carotene and soluble fibre in a format that is easier to digest than whole grains.
Lunch: Tuna salad made with lactose-free Greek yogurt and hard-boiled egg, served on plain crackers. Applesauce with cinnamon on the side.
Dinner: Salmon cakes with mashed potatoes and roasted carrots, using olive oil throughout. Mashed potatoes are one of the most universally tolerated starchy foods in UC.
Snacks: Chia pudding made with almond milk and cinnamon (small portion — chia seeds are high fibre, so monitor tolerance); banana with warmed peanut butter.
Day 4 — Balancing Nutrition and Tolerance
Breakfast: Smoothie with lactose-free milk or almond milk, banana, two tablespoons of peanut butter, unsweetened cocoa powder, and ground flaxseed. Smoothies allow nutritional density without requiring the digestive system to process whole food fibre structures.
Lunch: Quinoa salad with cooked and cooled quinoa, chopped cucumbers, tomatoes, and bell peppers, dressed with olive oil and lemon. Add cooked chicken for protein. Note — quinoa is higher fibre than white rice. If this causes symptoms, substitute white rice or remove and reassess.
Dinner: Three-bean chili with black beans, kidney beans, and pinto beans, diced tomatoes, garlic, and tomato paste, served with homemade cornbread. High fibre — monitor response carefully. If this is during active mild disease, reduce bean content and increase chicken or turkey.
Snacks: Hummus and plain crackers; walnuts (small portion — monitor tolerance during active disease) and pear applesauce.
Day 5 — Nutrient-Dense and Easily Digestible
Breakfast: Bean-based muffins (navy beans blended into banana muffin batter — provides protein and fibre in a tolerated format), with scrambled eggs.
Lunch: Leftover three-bean chili over a small baked potato topped with shredded cheddar if tolerated. Baked potato is among the most universally tolerated starchy foods in UC.
Dinner: Baked cod with white rice and cooked green beans or courgette, seasoned with olive oil, garlic, lemon, salt, and pepper. White fish is very easily digestible and an excellent lean protein source.
Snacks: Plain lactose-free nonfat yogurt; hard-boiled egg and plain crackers.
Day 6 — Comfort Foods with a Healthy Approach
Breakfast: Energy bites made with old-fashioned oats, chia seeds, peanut butter, unsweetened cocoa powder, pure maple syrup, and dark chocolate chips, paired with a small banana.
Lunch: Green smoothie with avocado, lactose-free milk (or almond milk), frozen banana, ground flaxseed, and white cannellini beans. Avoid high-insoluble-fibre vegetables in this smoothie if disease is not fully in remission.
Dinner: One-pot slow-cooker chicken with carrots and potatoes, seasoned with oregano, black pepper, salt, and parsley. Slow-cooked meals produce very tender, easily digestible vegetables and proteins — ideal for UC.
Snacks: Baked apples; Colby cheese and crackers if lactose is tolerated.
Day 7 — Variety and Classic Favourites
Breakfast: Microwaved old-fashioned oats with lactose-free milk, ground flaxseed, cinnamon, chopped walnuts, and cooked apples.
Lunch: A simple gut-friendly platter — water-packed tuna, hummus, plain crackers, black and green olives, and peaches or pears canned in water or juice.
Dinner: Mashed potato bowls topped with tender slow-cooked chicken or turkey, cooked garlic, green beans, and baked pears. Mashed potatoes with soft protein and cooked vegetables — one of the most reliably well-tolerated UC-friendly meals.
Snacks: Popsicles made from smoothie leftovers; peanut butter mixed into plain Greek yogurt.
Practical Tips for Managing Nutrition With UC
Eat smaller, more frequent meals — five to six small meals daily puts less mechanical stress on the colon than three large ones and maintains more consistent blood glucose and energy levels.
Keep a food and symptom diary — individual triggers vary enormously between UC patients. A systematic food diary is the most effective way to identify your personal triggers. Note every food eaten and any symptom changes over the following 24 hours.
Cook vegetables thoroughly — cooking breaks down cell walls and significantly reduces the fibre structure that can aggravate UC. Steaming, roasting, and slow-cooking all work well. Raw vegetables are better reserved for stable remission.
Peel fruits and vegetables — the skin of fruits and vegetables is high in insoluble fibre. Peeling before eating significantly reduces the fibre load.
Stay well hydrated — diarrhoea during UC causes significant fluid and electrolyte loss. Water, diluted fruit juice, and oral rehydration solutions are appropriate. Avoid caffeinated and carbonated beverages during flares.
Avoid eating late at night — the gastrocolic reflex — the urge to defecate triggered by eating — is strongest in the morning. Eating a large meal late at night can increase nocturnal symptoms.
Consider nutritional supplementation — given the nutrient depletions caused by UC itself and its medications, a daily multivitamin is reasonable for most UC patients. Specific supplementation for calcium, vitamin D, iron, folate, and B12 should be guided by blood test results and discussed with your physician.
When to Contact Your Doctor
Dietary management has limits. Contact your gastroenterologist if you experience:
- More than six bloody stools per day
- Significant abdominal pain not relieved by dietary changes
- Fever above 38°C / 100.4°F
- Unintentional weight loss of more than 5% of body weight
- Signs of severe anaemia — extreme fatigue, pallor, breathlessness
- Symptoms that are worsening despite dietary adjustments
These symptoms indicate a flare requiring medical assessment and potentially medication adjustment — not dietary intervention alone.
Frequently Asked Questions
What is the best diet for ulcerative colitis?
No single diet has been proven to consistently induce or maintain UC remission across all patients. The strongest clinical evidence supports: a Mediterranean-style anti-inflammatory eating pattern during remission, a low-residue low-fibre approach during active flares, avoiding ultra-processed foods and red and processed meats long term, and individually identifying and avoiding personal trigger foods through a systematic food diary.
What foods trigger ulcerative colitis flares?
The most consistently reported trigger foods across UC patients include spicy foods, raw high-fibre vegetables, nuts and seeds, alcohol, caffeine, carbonated beverages, dairy (in lactose-intolerant patients), sorbitol-containing sugar-free products, ultra-processed foods, and red and processed meats. Individual triggers vary — a food diary is the most reliable way to identify your personal triggers.
Can diet alone treat ulcerative colitis?
No — UC is a chronic immune-mediated disease requiring medical management. Diet is a critically important adjunct to medical therapy that can significantly improve quality of life, reduce symptom severity, and support remission maintenance. But diet cannot replace the medications used to manage UC, particularly during moderate-to-severe flares.
Is fibre good or bad for ulcerative colitis?
It depends on the type of fibre and the phase of disease. Soluble fibre — from oats, cooked carrots, peeled fruit, and psyllium — is generally well tolerated and supports gut microbiome health in UC. Insoluble fibre — from raw vegetables, whole grains, bran, nuts, and seeds — increases stool bulk and intestinal motility and typically worsens symptoms during a flare. During remission, gradual reintroduction of higher-fibre foods as tolerated is appropriate.
Should I take probiotics for ulcerative colitis?
Some evidence supports probiotic use in UC — VSL#3 (a high-potency multi-strain probiotic) has the strongest IBD-specific clinical evidence for remission maintenance in mild-to-moderate UC. Fermented foods including kefir and live-culture yogurt also support gut microbiome health. Discuss probiotic supplementation with your gastroenterologist before starting, particularly if you are on immunosuppressive therapy.
Can ulcerative colitis cause nutritional deficiencies?
Yes — frequently. Iron deficiency anaemia is the most common, affecting up to 74% of UC patients. Vitamin D, calcium, folate, vitamin B12, magnesium, and zinc deficiencies are also common — worsened by malabsorption during flares, medication depletions, and restricted eating. Regular blood monitoring of nutritional status is an important part of UC management. See our guide on Weight Loss Shots with B12 for context on B12 deficiency and supplementation.
Key Takeaways
- UC management requires a distinction between eating during a flare (low-residue, low-fibre, easily digestible) and eating in remission (gradually reintroducing variety, anti-inflammatory focus)
- The 2024 AGA Clinical Practice Update states a diet low in red and processed meat may reduce UC flares — avoiding ultra-processed foods and processed meats is the most evidence-based dietary recommendation for UC long term
- Corticosteroids deplete calcium, vitamin D, potassium, and magnesium — supplementation should be discussed with your physician during and after courses
- Azathioprine, 6-mercaptopurine, and mesalamine all reduce folate — adequate dietary folate and potential supplementation should be discussed with your physician
- Iron deficiency anaemia affects up to 74% of UC patients — if you are fatigued, pale, or breathless, ask for a full blood count and iron panel
- No diet has consistently been shown to induce UC remission across all patients — diet is a critically important adjunct to medical therapy, not a replacement
- Individual trigger foods vary significantly — a food and symptom diary is the most effective tool for identifying your personal triggers
References
- Herrador-López M, Martín-Masot R, Navas-López VM. Dietary Interventions in Ulcerative Colitis: A Systematic Review of the Evidence with Meta-Analysis. Nutrients. 2023;15(19):4194. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10574654/
- Abbas AM, et al. A Systematic Review of the Role of Diet in Ulcerative Colitis. Cureus. 2023;15(5):e39350. https://pmc.ncbi.nlm.nih.gov/articles/PMC10284595/
- Hashash JG, Elkins J, Lewis JD, Binion DG. AGA Clinical Practice Update on Diet and Nutritional Therapies in Patients With Inflammatory Bowel Disease. Gastroenterology. 2024;166(3):521–532. https://pubmed.ncbi.nlm.nih.gov/38276922/
- Reznikov EA, Suskind DL. Current Nutritional Therapies in Inflammatory Bowel Disease. Nutrients. 2023;15(3):668. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9920576/
- Calder PC. Omega-3 fatty acids and inflammatory processes. Biochemical Society Transactions. 2017. https://pubmed.ncbi.nlm.nih.gov/28900017/
- Crohn’s and Colitis UK. Food and IBD — Patient Information. Crohn’s and Colitis UK. https://crohnsandcolitis.org.uk/media/klqnlo0j/food-ed-9-2023-leaflet.pdf
- NHS. Ulcerative colitis — living with. National Health Service. https://www.nhs.uk/conditions/ulcerative-colitis/living-with/